Occupational Therapy Role in Flexor Tendon Injury
by Dr. Arun Kumar
INTRODUCTION:
A flexor tendon injury is a damage to the tendons that allow you to bend your fingers, thumb, and wrist. These tendons are long, cord-like structures that run from the muscles in your forearm to the bones in your fingers and thumb. When a flexor tendon is injured, you may lose the ability to bend one or more of your fingers or your thumb.
TYPES:
There are two main types of flexor tendon injuries:
Lacerations: These are cuts to the tendon, which can be caused by knives, glass, or other sharp objects.
Ruptures: These are tears in the tendon, which can be caused by overuse, sudden trauma, or a forceful blow to the hand.
CAUSES:
DIRECT TRAUMA
Lacerations: This is the most common cause, with cuts from knives, glass, power tools, and other sharp objects severing or damaging the tendon.
Crush injuries: Pinching or crushing the finger between heavy objects can damage the tendon.
Bites: Animal bites, especially from dogs or cats, can puncture and tear the tendon.
Fractures: Displaced bone fragments can damage nearby tendons during a fracture.
OVERUSE AND REPETITIVE STRAIN
Sports activities: Certain sports like football, basketball, and wrestling put repetitive stress on the tendons, increasing the risk of tears or ruptures.
Manual labor: Jobs involving repetitive gripping, forceful movements, or heavy lifting can lead to tendon irritation and inflammation, eventually weakening and causing tears.
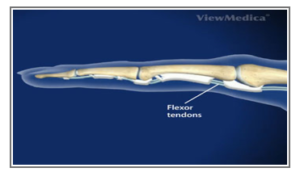
SYMPTOMS:
Difficulty bending one or more fingers
or your thumb
Pain at the site of the injury
Swelling
Numbness or tingling
Deformity of the finger or thumb
TREATMENT:
The treatment for a flexor tendon injury depends on the severity and type of injury, but typically involves a combination of the following:
IMMEDIATE CARE:
Immobilization: Splinting or casting the hand and fingers to rest and protect the injured tendon.
Pain management: Medication to manage pain and inflammation.
Wound care: If there’s a laceration, proper cleaning and wound care are crucial to prevent infection.
SURGERY
Tendon repair: This is the most common treatment for severe injuries involving complete or partial tendon tears. Surgery aims to reattach the torn ends of the tendon and restore its function.
Tendon tenolysis: In some cases, scar tissue buildup around the tendon sheath can restrict movement. Surgery to remove scar tissue (tenolysis) may be necessary to improve finger flexion.
OCCUPATIONAL THERAPY INTERVENTION:
Education and Pain Management: OTs educate patients about their injury, the healing process, and expected outcomes. They also provide strategies for managing pain and edema to facilitate participation in therapy.
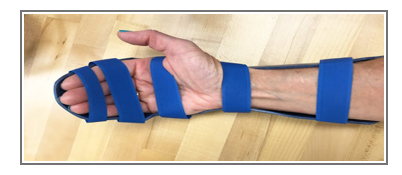
Splint Customization and Training: OTs can customize splints for optimal hand positioning and support during different stages of healing.
They also train patients on safe splint use and removal, promoting self-management.
Scar Management: OTs use scar massage, pressure therapy, and other techniques to prevent excessive scar tissue formation, which can impact tendon gliding and finger movement.
FUNCTIONAL REHABILITATION:
Activities of Daily Living (ADL) Training:
OTs assess and address limitations in performing daily tasks like dressing, grooming, and bathing. They provide adaptive equipment and strategies to modify activities and promote independence.
Work Reintegration: For individuals returning to work, OTs evaluate job demands and adapt tools or workstations to accommodate limitations. They also train on safe work practices to prevent reinjury.
Sensory Retraining: After surgery, some patients experience altered sensation in their fingers. OTs use sensory stimulation techniques to improve tactile awareness and proprioception, crucial for fine motor control.
SPECIFIC TECHNIQUES
Joint Mobilization and Stretching: Gentle manual techniques are used to improve joint mobility and prevent contractures (stiffness) in the fingers and wrist.
Strengthening Exercises: Gradual progressions of exercises are designed to increase finger and hand strength, essential for regaining functional hand use.
Fine Motor Activities: OTs incorporate tasks like handwriting, buttoning, and using tools to improve dexterity and coordination in daily activities.
Cognitive Strategies: OTs may use cognitive-behavioral approaches to address pain, anxiety, and fear associated with hand use, promoting motivation and engagement in therapy.
